


Surgical videos are essential educational tools for vitreoretinal surgeons. The ability to rapidly share innovative surgical procedures with colleagues via video has made a positive impact on both surgical education and patient care. In the past, surgical procedures were mostly taught through photographic illustrations accompanied by descriptive narratives or in surgical theaters, where less experienced surgeons learned through direct observation and participation. Increased utilization of video technology has facilitated expeditious communication among ophthalmic surgeons and the practical demonstration of complex surgical manipulations.
AT A GLANCE
• Video technology has become an important component of medical and surgical education.
• 4K is a viewing platform with a horizontal resolution of at least 4,000 pixels, four times the resolution of full HD (1,080 pixel) technology.
• Devices with 4K resolution present a new frontier in video technology, providing excellent resolution of fine intraocular structures.
Video technology itself has undergone significant advances in recent years. The optical resolution of digital cameras and display monitors has steadily improved, resulting in enhanced ability to capture and view high-quality surgical videos. The inefficient processes of transferring and storing analog tapes have been replaced by simplified processes of storing and sharing digital files. Additionally, digital technology has made the recording and editing of surgical videos straightforward tasks that can easily be adopted by every retina surgeon.
High quality display monitors have now begun to play a vital role in the OR, demonstrating the real-time progress of a surgical case, facilitating communication between surgeons and OR staff, and improving the flow of operating procedures. Indeed, the educational value of video technology has increasingly been recognized.1,2 Surgical videos have become not only an indispensable part of medical education but also important tools for improving patients’ understanding of their medical conditions.3
This article reviews some recent improvements and remaining hurdles of high-resolution video technology and offers insights on how the latest technology, 4K, can benefit our profession.
IMPROVEMENTS IN VIDEO TECHNOLOGY
Resolution
The resolution of digital video technology is rapidly improving. High-definition (HD) video (any video image with >480 horizontal lines) has become widely available, providing clearer and sharper images compared with standard definition video.4 Nevertheless, current HD technology offers significantly higher resolution, with 1,080 horizontal lines, or 1,920 x 1,080 pixel image resolution (full HD), which is the industry standard.
Watch it Now
4K Ultrahigh-Definition Video Taken During a Vitrectomy
The video demonstrates high image quality and sharper structural details. Authors’ note: The true quality of this video can be appreciated only on a 4K monitor. When viewed on a regular computer monitor the image quality is only as good as the monitor itself.
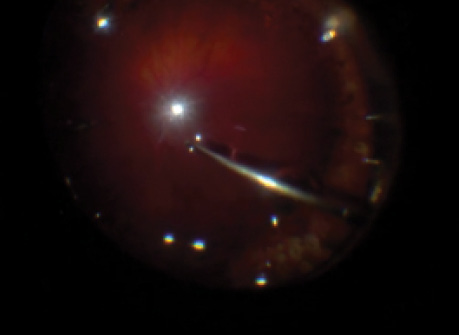
The surgery began with removal of silicone oil using a 25-gauge vitrectomy system. Several air-fluid exchanges were performed to wash out the residual silicone bubbles. Indocyanine green was used to stain the epiretinal membrane (ERM). The ERM flap was initiated and the membrane was peeled. Fine structural details of the ERM, such as surface folds, were clearly visible on the 4K monitor. Air-fluid exchange was performed and the trocars were removed. Light external diathermy was applied to seal sclerotomy wounds, which concluded the surgery.
4K Technology
Another recent advancement in high-resolution video has been the introduction of 4K technology. 4K resolution, or simply 4K, is a viewing platform with a horizontal resolution of at least 4,000 pixels (3,840 x 2,160 pixels). This means that 4K has four times the resolution in pixels compared with 1,080 technology, which translates into four times superior image detail, allowing identification of fine structures with greater precision. 4K technology is highly suitable for use with ophthalmic operating microscopes.
The advanced optical systems of modern ophthalmic surgical microscopes permit incorporation of 4K imaging devices without any compromise in image resolution. To date, this is not the case with surgical endoscopes, which are at this time unable to handle resolution capabilities higher than full HD. The incorporation of high-resolution image technology into surgical microscopes is being explored, and the future of this technology holds promise for transforming ophthalmic microsurgery.
VIDEO TECHNOLOGY: MEDICAL VS. CONSUMER
Unlike consumer devices, medical devices are required to undergo stringent safety evaluation by the US Food and Drug Administration and must be specifically labeled for their intended uses.
Consumer video devices are designed to make video images more bright, brilliant, and colorful in order to enhance the image quality and the viewer’s experience for their intended use (eg, watching movies, playing video games). Conversely, display monitors used for medical purposes are designed to accurately and realistically demonstrate the appearance of observed structures and limit image variability between frames.
FEEDBACK FROM PROFESSIONAL EXPERIENCE
Recently, our retina surgical team had an opportunity to use 4K video technology in our OR for a variety of cases, including diabetic retinal detachments and macular cases. We used consumer devices because medical 4K devices were not yet commercially available in the United States. We used the a7s 4K digital full frame camera (Sony) with 4K video output over HDMI connections as a source, with a specially made TTI 4K lens adapter connected to our Opmi Lumera 700 microscope (Carl Zeiss Meditec). The video was recorded to a Convergent Design Odyssey 7Q+ 4K recorder, and the files were saved in Apple ProRes HQ 422 format. Live 4K video was presented to OR personnel on a 49-inch 4K consumer television screen (Sony).
Image quality and discernible structural details were impressive (Video). All ocular structures were significantly in sharper focus and their details were more easily observed. For example, we were able to appreciate fine details such as mild folds on the surface of the epiretinal membrane that we could not visualize on a regular monitor.
The future of this technology appears quite promising. Medical products with 4K capabilities will be specifically designed for use in the OR. A 4K camera attached to a surgical microscope is expected to become available in the near future. Combining 3-D technology with 4K technology has the potential to eliminate binoculars from surgical microscopes and lead to higher quality heads-up surgical platforms than those currently available for ophthalmic surgery. Beyond 4K, 8K resolution has rapidly been developing and is currently the highest resolution format for digital television. Typically, when pixel size is increased, light sensitivity is decreased; however, new technologies have addressed this issue to some extent.
CURRENT AND ANTICIPATED OBSTACLES
Size and Cost
Despite improvements in resolution, current HD video technology has some drawbacks. As the technology itself evolves, the amount of data gathered increases exponentially. It is also important to note that 4K video files are large and difficult to store, play, and transfer on less powerful computer devices. Large files can be compressed into smaller files, but it is difficult to do this without losing resolution and image quality.
Similarly, editing of 4K video files can be cumbersome and may take a long time when done on a regular computer. Currently available 4K editing software (eg, Sony Vegas Pro, Adobe Premiere Pro, and Apple Final Cut Pro) is expensive. In fact, 4K devices in general are significantly more expensive than full HD devices; however, the cost is expected to drop as the technology becomes more widely available.
Latency
As the prospect of heads-up ophthalmic surgery becomes more feasible, a well-recognized hurdle is the visual delay, or latency, inherent to electronic devices. Each device in the imaging chain has its own latency period that contributes to the final cumulative latency observed on display monitors. The latency achieved by current technology is less than 100 ms and actually closer to 75 ms in advanced recording systems.
The phenomenon of latency is well documented in laparoscopic and robotic surgery.5 Experienced laparoscopic surgeons learn to compensate for this latency. However, the potential downside of latency in delicate macular surgery is theoretically more challenging to overcome because it affects a surgeon’s ability to work on delicate tissue, such as when peeling internal limiting membrane or epiretinal membrane (movement already occurs by the time it is visible on the screen). Heads-up visualization systems have been used successfully in many institutions for all types of retinal surgeries, including macular surgery, and this latency does not seem to present a real problem. The TrueVision 3D Surgical system (TrueVision 3D Surgical), introduced in 2008, uses a standard high-definition monitor. Alcon’s Ngenuity 3D Visualization System, developed in collaboration with TrueVision 3D Surgical and launched this September, features a 4K monitor and is used in heads-up surgery.
WORKING OUT THE KINKS
Cutting-edge video technology has become an important component of medical and surgical education. Surgical videos are excellent tools for sharing innovative techniques with vitreoretinal colleagues. Devices with 4K resolution present a new frontier in video technology and provide excellent resolution of fine intraocular structures. As the technology evolves, current limitations will be overcome and systems will become more affordable. Commercial 4K medical devices (eg, the Ngenuity 3D Visualization System), have recently become available for vitreoretinal surgery in the Unites States. n
1. Dinscore A, Andres A. Surgical videos online: a survey of prominent sources and future trends. Med Ref Serv Q. 2010;29(1):10-27.
2. Prinz A, Bolz, Findl O. Advantage of three dimensional animated teaching over traditional surgical videos for teaching ophthalmic surgery: a randomized study. Br J Ophthalmol. 2005;89(11):1495-1499.
3. Hoppe DJ, Denkers M, Hoppe FM, Wong IH. The use of video before arthroscopic shoulder surgery to enhance patient recall and satisfaction: a randomized-controlled study. J Shoulder Elbow. 2014;23(6):e134-139.
4. Conrad J, Philipps M, Oertel J. High-definition imaging in endoscopic transsphenoidal pituitary surgery. Am J Rhinol Allergy. 2011;25(1):e13-17.
5. Kim T, Zimmerman PM, Wade MJ, Weiss CA 3rd. The effect of delayed visual feedback on telerobotic surgery. Surg Endosc. 2005;19(5):683-686.
Denis Jusufbegovic, MD
• assistant professor of ophthalmology, Indiana University School of
Medicine, Indianapolis, Ind.
• financial interest: none acknowledged
• d0jusu01@gmail.com
Agustina Palacio, MD
• research fellow in the department of ophthalmology and visual
sciences, University of Louisville, Ky. • financial interest: none acknowledged
• aguspalacio@gmail.com
Shlomit Schaal, MD, PhD
• professor and chair of the department of ophthalmology and
visual sciences, University of Massachusetts Medical School,
Worcester, Mass.
• financial interest: none acknowledged
• s.schaal@umassmed.edu











_1773249222.png?auto=compress,format&w=75)










