In a 2016 article in New Retina MD entitled “The Next Chapter: Forging a Concept of International Retinal Care,” I wrote about the task of crowdsourcing the answers to two central questions. First, what should be the primary goals for vitreoretinal surgeons interested in engaging on an international scale? Second, what are the most responsible, effective, and sustainable means of achieving those goals? In search of detailed answers, I recently reached out to two vitreoretinal surgeons with strong résumés of international involvement to ask for their insights on how to build networks for screening for retinal disease in underserved areas.
Benjamin J. Thomas, MD: Ophthalmology has a broad history of working internationally and delivering care across multiple cultural and economic contexts, but a uniting concept of international retina remains relatively new. How would you define the primary interests, tasks, and goals of international retina?
Eric D. Hansen, MD: 12.5 million people are blind or severely visually impaired due to AMD and diabetic retinopathy alone.1 Another significant proportion of visual impairment, hidden in the broad strokes of global surveys, falls within the scope of vitreoretinal care. Diseases such as myopic degeneration, uveitis, oncology, trauma and its sequelae, toxicity, surgical complications, and inherited disease all contribute to the more than 200 million people worldwide with (as yet) uncharacterized visual impairment.
The task presented to the international retina community is understanding policy and public health principles and applying this understanding to a highly specialized field that provides high-acuity care while also treating chronic disease within a coordinated, multidisciplinary paradigm.
This task, as expressed, is admittedly daunting. Individuals and organizations working within this space must rely on a broad history of global ophthalmology initiatives—both the successes and failures—to present an organized, prioritized, adaptable blueprint for integrating medical and surgical retinal care into a universal eye health system.
This model will differ from that which has been successful in the realm of cataract blindness. Here, the timing of presentation influences outcomes considerably. Additionally, availability for frequent follow-up alongside reliable access to consumables and specialized therapeutics is requisite for the success of international retina.
Dr. Thomas: What prompted your own interest in international retinal work, and with what projects have you had the opportunity to be involved?
Dr. Hansen: I am not sure I can identify a particular prompt. Life and calling unfold as a story—a river of opportunities and decisions that empty into one’s present. I see the interconnectedness of humanity and of life on this planet in a way that drives me to invest energy in a common future. So, with this perspective as an anchor, and a roster of incredible mentors as a catalyst, I waded into the world of global health as a medical student and immersed myself in the community of international ophthalmology following residency. I have worked with the Moran Eye Center and the Himalayan Cataract Project for more than 4 years—first as a global ophthalmology fellow then onward through vitreoretinal training—in their efforts to build capacity locally in Utah and in other parts of the world.
Christopher B. Komanski, MD: I was fortunate to complete my residency at a program with a global outreach division at Wake Forest. My first hands-on experience was performing cataract surgery in San Pedro Sula with Tim Martin, MD; Matt Giegengack, MD; and Paul Dickinson, MD. The experience was impactful, and it motivated me to look for opportunities to apply my retina training in a similar way. During fellowship, I worked with incredible mentors such as Paul Bernstein, MD, PhD; Akbar Shakoor, MD; and Al Vitale, MD, who have all made tremendous contributions to international retina and uveitis.
BARRIERS TO CARE
Dr. Thomas: Considering the endeavor of international retina from both a personal perspective and a more global context, what are the primary barriers you perceive to the delivery of retinal care in resource-poor settings?
Dr. Hansen: Common barriers include patient access due to geography or distance; cost of treatment for the patient and cost of consumables for the hospital; procurement and maintenance of equipment; and the maintenance of a reliable supply chain of necessary pharmaceuticals, consumables and instruments. In addition, vitreoretinal training opportunities are limited. And even when identified and available, there is often a significant opportunity cost associated with an ophthalmologist leaving a community for 1 to 2 years to train.
Dr. Komanski: Patient expectations and how they align with cultural barriers; the need for frequent follow-up in chronic disease; the importance of timing in presentation and its influence on outcomes, especially compared with cataracts—to name a few.
Dr. Hansen: Medical retinal care, in particular, requires integration with primary care and other medical specialties. Often, we are fighting a losing battle if we cannot address or control the underlying pathology.
Dr. Thomas: Mature cataracts can be diagnosed with minimal dilation and a flashlight. Not so for retinal diseases, such as diabetic retinopathy, which usually require advanced techniques, equipment, and training to detect. How does this aspect of retinal care change our strategy for expanding into new or underserved regions?
Dr. Komanski: Imagine a hub-and-spoke model, with screening programs established in underserved communities that integrate primary care systems or community health workers with a center of excellence employing retina-trained physicians. After screening and disease confirmation, intervention may be organized by the center of excellence to be carried out in any number of locations, including the hub, a peripheral referral center, or even in more rural sites depending on the type and severity of disease and the appropriate intervention.

Dr. Komanski joined an international team of providers to bring much-needed eyecare to underserved patients in San Pedro Sula, Honduras.
Dr. Hansen: It’s important to recognize that great models exist that are worth emulating, including Aravind in India, various US telehealth systems, and a mobile diagnostic program that was studied in Nepal.2 Ophthalmology-extending mechanisms, such as ophthalmic technicians and trained community health workers using mobile diagnostics, are also great tools, but each must be tailored for use within specific geographic and socioeconomic contexts.
Dr. Komanski: Mobile diagnostics and other technologies can empower community health workers, primary care physicians, optometrists, and cataract surgeons, thereby expanding the network of caregivers involved in vitreoretinal work.
Dr. Hansen: Difficulties still exist with solving the problems of costly treatments and arduous travel. In the United States, we solve the problem of dispersed populations by having physicians travel to these communities at regular intervals. Why can’t we do this internationally?
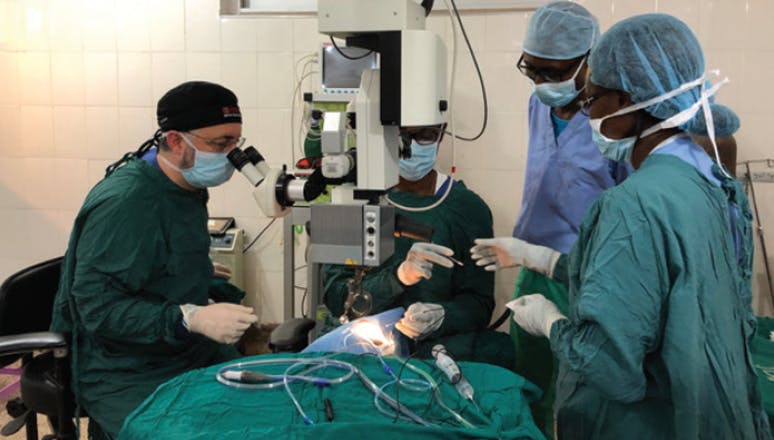
Dr. Bernstein proctors as Akwasi Ahmed, MD, performs the first vitreoretinal surgeries in Kumasi, Ghana, at the Komfo Anokye Teaching Hospital. Supported by the Himalayan Cataract Project and Moran Eye Center, Dr. Ahmed completed vitreoretinal fellowships at Tilganga Insitute of Ophthalmology in Nepal and Aravind Eye Hospital in India. In 2018, Dr. Bernstein and Dr. Hansen traveled to Ghana for hospital-based, in-country training to support Dr. Ahmed’s role as the first vitreoretinal surgeon in the Kumasi region.
Mobile vision vans (or boats) with injection and laser capabilities, traveling at regular intervals to surrounding communities, can be a great way to bring modern medical retina therapeutics to more patients. For example, the Moran Eye Center partners with the Federation of Micronesia and the sole ophthalmologist in the country to expand his capacity for providing ophthalmic care in his country. Micronesia is a country composed of hundreds and hundreds of islands reachable only by boat. Obviously, the calculus is not tilted in his favor. However, by training nurses and community health workers on individual islands to perform screenings, and equipping a team traveling from island to island by boat with interventional capacity, we can begin to reach Micronesians where they live and address their overwhelming need for diabetic eye care.
BUILDING A FOUNDATION
Dr. Thomas: What would you list as the core elements of a high-quality retinal screening program?
Dr. Hansen: This comes down to three As: awareness, access, and accountability. Awareness includes advertising and dissemination of information within the context of an individual community. Access requires established avenues for providing necessary follow-up and care. Accountability means we should not just study disease, but study outcomes and the effects of a given program. Don’t just identify problems, solve them; don’t just start a project, sustain it.
Dr. Thomas: What are the relative advantages and disadvantages of a specific screening program (eg, one focused on diabetic retinopathy) versus a more general screening strategy?
Dr. Hansen: Focused screening offers simplicity. Broadening a screening strategy will likely identify additional treatable diseases, but it also inflates and complicates the concurrent obligations of providing additional mechanisms of treatment. A strong screening and treatment algorithm for a common retinal disease, such as diabetic retinopathy, facilitates a goal-directed, high-impact program.
Even with a specific screening strategy focused on a single disease entity, it is likely that many other retinal pathologies will also be identified in the course of screening. This may offer important epidemiologic information and provide direction for future work in the region. It also impels an organization to have a plan for addressing this reality.
Dr. Thomas: How can technology aid us in expanding screening and detection efforts, particularly in resource-poor settings? What have we learned recently about low-cost techniques and technologies for detecting retinal disease, and how might they work if employed on a large scale?
Dr. Komanski: I think technology has immense potential to expand the detection and monitoring of retinal disease in resource-poor and geographically remote settings. For instance, the development of the RETEval DR (Welch Allyn), a low-cost electroretinogram to detect vision-threatening diabetic retinopathy, is particularly exciting as it allows rapid screening of at-risk patients unable to undergo a formal eye exam. I imagine some combination of this with a nonmydriatic widefield imaging system, such as the Zeiss Clarus or Optos, as a means of allowing retina specialists to remotely confirm high-risk diabetic retinopathy. But I also hesitate to elevate these technologies as a panacea, given that they do little to remove barriers to delivery of care on the back end. They must be employed within an organized and prioritized framework that addresses both sides of the equation.
1. Adelson J, Bourne RRA, Briant PS, et al. Causes of blindness and vision impairment in 2020 and trends over 30 years: evaluating the prevalence of avoidable blindness in relation to “VISION 2020: The Right to Sight”. The Lancet Global Health. 2020. [In press]
2. Collon S, Chang D, Tabin G, Hong K, Myung D, Thapa S. Utility and feasibility of teleophthalmology using a smartphone-based ophthalmic camera in screening camps in Nepal. Asia Pac J Ophthalmol. 2020;9(1):54-58.












_1773249222.png?auto=compress,format&w=75)












