Diabetes is a growing epidemic, with one in every 10 people living with diabetes worldwide1; in many countries, the number reaches upwards of 30% of the population—and is growing.1 More than 50% of patients with type 1 diabetes and 25% with type 2 diabetes will develop diabetic retinopathy (DR),2 which can lead to other vision-threatening complications, such as vitreous hemorrhage or tractional retinal detachment. Up to 20% of those people will develop diabetic macular edema (DME), which is possible at any stage of DR.2 While anti-VEGF injections can be a good treatment approach for DME, regular access to anti-VEGF therapy can be a significant challenge for many patients.
AT A GLANCE
- The role of vitrectomy for diabetic macular edema is controversial because studies show anatomical but not functional improvement; however, those results may be due to patient selection criteria.
- Long-standing macular edema results in irreversible changes to retinal tissue, especially photoreceptors, making it nearly impossible to achieve visual improvement if treatment is delayed.
- The cost of vitrectomy may be favorable compared with multiple injections for the treatment of diabetic macular edema.
The role of vitrectomy in the treatment of DME is controversial. Many studies found anatomical but not functional improvement with this approach.3 However, those results might be due, in part, to the patient selection criteria (ie, we usually decide on surgical treatment when all other available methods, such as laser treatment, anti-VEGF agents, and steroid injections, have failed).4
Long-standing DME results in irreversible changes to retinal tissue, especially photoreceptors, making it nearly impossible to achieve visual improvement with delayed treatment. We published a study on treatment-naïve patients who qualified for vitrectomy with internal limiting membrane (ILM) peeling and reported a stable 3-line improvement in visual acuity for 55% of patients, with only 8% of eyes worsening by 1 line in the 48-month postoperative period (Figure 1).5 We hypothesize that these excellent results, which differ significantly from many previous studies, were associated with our inclusion criteria. We included patients with relatively well-controlled diabetes (mean hemoglobin A1c levels were 7.5%) with no prior laser photocoagulation in the macula region, nor anti-VEGF therapy.

Figure 1. Swept-source OCT shows DME before vitrectomy in a 63-year-old woman (A). Postoperatively, OCT imaging of the same patient shows resolution of the DME (B).
UNMET NEEDS
Today's standard treatment approach for DME is continuous anti-VEGF injections. Although they improve vision and reduce central retinal thickness, they require frequent administration, can be costly, and are not ideal for all patients with diabetes.
Diabetic complications beyond DME often hinder patients' ability to maintain a regular dosing schedule. Systemic concerns, such as kidney disease (leading to dialysis or lower limb amputations), peripheral nerve disease, depression, and many other comorbidities can limit patients' communication, mobility, and ability to appear for regular, ongoing, injections, leading to significant loss to follow-up. In fact, patients with diabetes are more likely to drop out from treatment than other patient population.6
As for the financial ramifications, rebates and other assistance programs for anti-VEGF treatment are available in developed countries for insured individuals. Still, more than half of the world's population does not have access to these drugs—creating the need for other accessible and cost-effective therapies.
Anti-VEGF drugs are teratogenic and are contraindicated in individuals who are pregnant or are planning pregnancy. Those in this group who have type 1 diabetes and have developed DME are already on regular long-term treatment. Because they are usually phakic, intraocular steroids are rarely a viable treatment option.
A NOT-SO-NOVEL APPROACH
Vitrectomy may be the answer to these needs. The clear advantage of surgical treatment is a low recurrence rate (less than 15% during a 10-year observation period).7 Recurrences of DME are often associated with worse diabetes control but are generally easy to handle with single anti-VEGF injections.
In addition, the cost of a single surgery may be favorable compared with multiple injections. In an important comparative study of patients treated with anti-VEGF agents in the better-seeing eye and vitrectomy in the worse-seeing eye, the long-term visual benefit was identical between eyes.8 Moreover, time to recovery was not statistically significant. The progression of disease and fluctuating levels of hemoglobin A1c could significantly influence treatment outcomes, making the conclusions of this study particularly valuable. Both eyes had identical baseline characteristics and identical systemic disease control for the duration of the study.
Vitrectomy can remove traction, improve oxygenation, and remove growth factors trapped at the retinal surface by the adherent posterior hyaloid.
DR does not always develop concurrently with vision loss caused by DME. Research suggests that the foveal avascular zone (FAZ), visualized with OCT angiography (OCTA), increases with DR progression.9 Anti-VEGF treatment can have a protective role against the progression of DR, and, using swept-source OCTA, we found that the FAZ decreases after vitrectomy (Figure 2).10,11 These data suggest an additional benefit of vitrectomy, in that it can reduce macular edema and improve vision. Thus, the reduction of the FAZ might play a protective role against the progression to more advanced stages of DR.
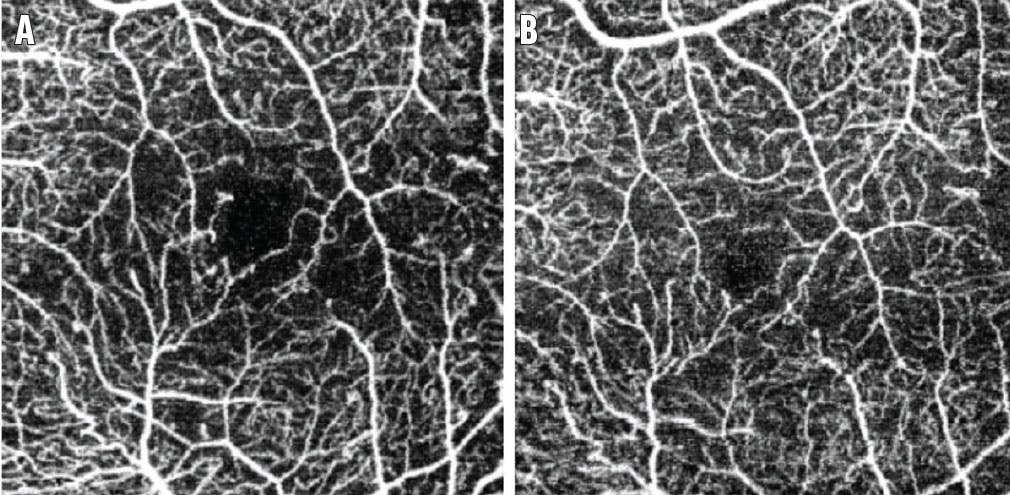
Figure 2. Swept-source OCTA of the eye of a 31-year-old patient before (A) and 4 months after vitrectomy (B). A decrease was observed in the FAZ in the superficial retinal vessel layer.
CLINICAL PEARLS
Vitrectomy may be a good choice and results in satisfactory long-term visual outcomes for patients with early disease. It may also be a good choice for patients with transportation difficulties, limited access to health care, and those planning pregnancy. The possible protective effect of vitrectomy against DR complications may be an added benefit.
1. Teo ZL, Tham YC, Yu M, et al. Global prevalence of diabetic retinopathy and projection of burden through 2045: systematic review and meta-analysis. Ophthalmology. 2021;128(11):1580-1591.
2. Li JQ, Welchowski T, Schmid M, et al. Prevalence, incidence and future projection of diabetic eye disease in Europe: a systematic review and meta-analysis. Eur J Epidemiol. 2020;35(1):11-23.
3. Simunovic MP, Hunyor AP, Ho IV. Vitrectomy for diabetic macular edema: a systematic review and meta-analysis. Can J Ophthalmol. 2014;49(2):188-195.
4. Flaxel CJ, Edwards AR, Aiello LP, et al. Factors associated with visual acuity outcomes after vitrectomy for diabetic macular edema: diabetic retinopathy clinical research network. Retina. 2010;30(9):1488-1495.
5. Michalewska Z, Stewart M, Landers MB, Bednarski M, Adelman RA, Nawrocki J. Vitrectomy in the management of diabetic macular edema in treatment naïve patients. Can J Ophthalmol. 2018;53:402-407.
6. Sam-Oyerinde OA, Patel PJ. Real-world outcomes of anti-VEGF therapy in diabetic macular oedema: barriers to treatment success and implications for low/lower-middle-income countries. Ophthalmol Ther. 2023;12(2):809-826.
7. Michalewska Z, Nawrocki J. Repeated surgery in primary failed vitrectomy for macular holes - a comparative study of primary classical ILM peeling vs. primary inverted ILM flap technique. Ophthalmic Surg Lasers Imaging. 2018;49(8):611-618.
8. Nawrocka ZA, Nawrocka Z, Nawrocki J. Vitrectomy with ILM peeling in diabetic macular edema in one eye vs. intravitreal anti-VEGF injections in the second eye: a comparative study. Graefes Arch Clin Exp Ophthalmol. 2023;261(1):67-76.
9. Freiberg FJ, Pfau M, Wons J, Wirth MA, Becker MD, Michels S. Optical coherence tomography angiography of the foveal avascular zone in diabetic retinopathy. Graefes Arch Clin Exp Ophthalmol. 2016;254(6):1051-1058.
10. Waisbourd M, Goldstein M, Loewenstein A. Treatment of diabetic retinopathy with anti-VEGF drugs. Acta Ophthalmol. 2011;89(3):203-207.
11. Nawrocka ZA, Nawrocki J. Vitrectomy in diabetic macular edema - a swept-source optical coherence tomography (OCT) angiography study. Ophthalmol Sci. 2022;9;2(4):100207.














_1773249222.png?auto=compress,format&w=75)










